Queens Councilman Francisco Moya hosted a COVID-19 virtual town hall with Elmhurst Hospital’s leadership on Monday, March 30, where they answered some of the community’s pressing questions and provided updates on the hospital’s needs.
The town hall featured a few words from Israel Rocha, vice president of NYC Health + Hospitals and CEO of Elmhurst and Queens Hospitals, and a presentation and Q&A with Dr. Joseph Masci, chairman of Elmhurst Hospital’s Department of Global Health and a specialist in general infectious diseases and emergency preparedness.
“A few years ago, Elmhurst [Hospital] realized that we actually were battling conditions, diseases and pathogens from all over the world, and that disease does not respect borders, it does not respect barriers,” Rocha said.
Rocha added that Elmhurst Hospital was one of the first hospitals in the country to create a Global Health program, which is led by Dr. Masci.
Dr. Masci noted that Elmhurst Hospital, which is now the epicenter of the pandemic in New York City, had 200 patients with COVID-19 as of Monday, March 30. “The hospital is very, very full right now,” he said.
He said that while they have the equipment and staff members they need, what they really need is space. If people want to donate nearby space or equipment, they should get in contact with Rocha or the hospital’s administration.
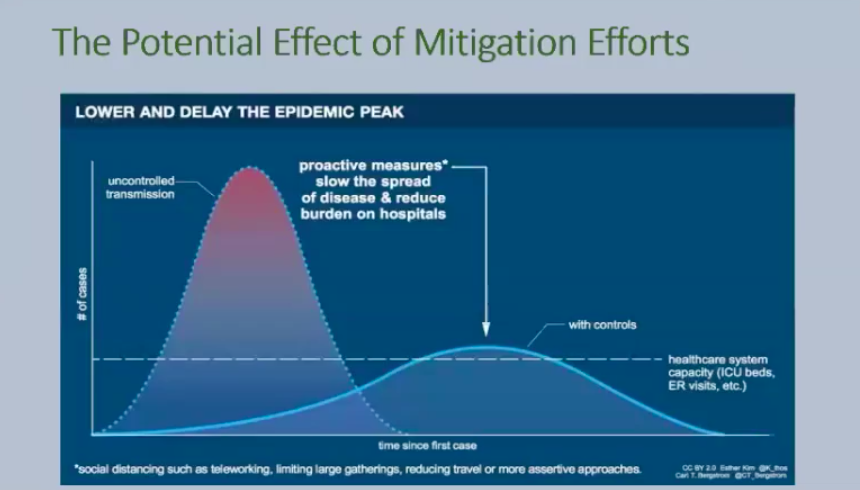
The peak of COVID-19 will see 30 to 40 percent more cases than there currently are in the city, according to Dr. Masci.
When asked why Queens and Elmhurst Hospital have been overrepresented in New York City’s COVID-19 health emergency, Dr. Masci said that while they can’t know anything until they have time to study it, the rest of New York City’s hospital system is now seeing similar activity.
“That initial spike in Queens is now being matched throughout the city,” he said.
Dr. Masci delineated some of what they’ve observed of COVID-19.

According to Dr. Masci, 80 percent of people who are infected have no symptoms or have symptoms that aren’t severe enough to require hospitalization, but 20 percent do require hospitalization. Five percent of that total will need intensive care.
Dr. Masci said that it’s uncommon for people under 30 to develop serious symptoms, according to cases around the world and in the U.S.
The Department of Health and Mental Hygiene strongly recommends against testing people with mild or no symptoms. But an indicator that individuals should go to the hospital is when they experience shortness of breath, Dr. Masci said.
When it comes to masks, Dr. Masci said that they won’t necessarily do anything to protect you if you’re not sick. He stressed that washing your hands more times than you think you should and staying home will minimize the risk of getting the virus.
Personal protective equipment, Dr. Masci said, should be preserved for hospital and medical employees. “We have to protect people who work in the hospitals, because if we lose them, then we’ll have a much bigger problem,” he said.
He also offered a look at what the future will bring.
He said it’s almost certain there will be many additional cases and deaths in the city and country, as well as confusing messages. They predict there will be further restrictions on travel in and outside of the country, more hospital crowding, and more hospital supply issues.
“We don’t think we’ve seen the peak of this yet. We think it’s going to continue to get worse for several more weeks,” Dr. Masci said.
Moya, who was born at Elmhurst Hospital and later worked there, thanked all the nurses, doctors, janitors and hospital workers for “doing God’s work.”
“We’ve been hit hard by this, but we’re New Yorkers. We’re resilient. We stick together. We band together, and if we do things right, we will get through this,” Moya said. “And I hope that tonight’s presentation will calm a lot of the fears and answer some of the questions we had here today.”
For more information, visit nyc.gov/coronavirus, and to reach Councilman Moya, email m21@council.nyc.gov.
To watch the full town hall, visit Councilman Moya’s Facebook page. A Spanish-translated version will be uploaded to YouTube.